Dog Hip Dysplasia: 6 Essential Facts Every Owner Should Know
Your large-breed dog has started moving differently. Maybe the morning stiffness is taking a little longer to work out, or the stairs that used to be effortless now get a wary glance. If your veterinarian has mentioned the words “hip dysplasia,” you’ve likely spent time since then sorting through dense medical descriptions that don’t quite answer the practical questions you’re facing.
This guide is built around six facts that change how owners understand and manage dog hip dysplasia — not abstractions, but the kind of information that shapes decisions about diagnosis timing, conservative versus surgical care, and daily home routines.
Fact 1: Hip Dysplasia Is a Structural Mismatch, Not a Single Disease
Hip Joint Anatomy and How Dysplasia Develops
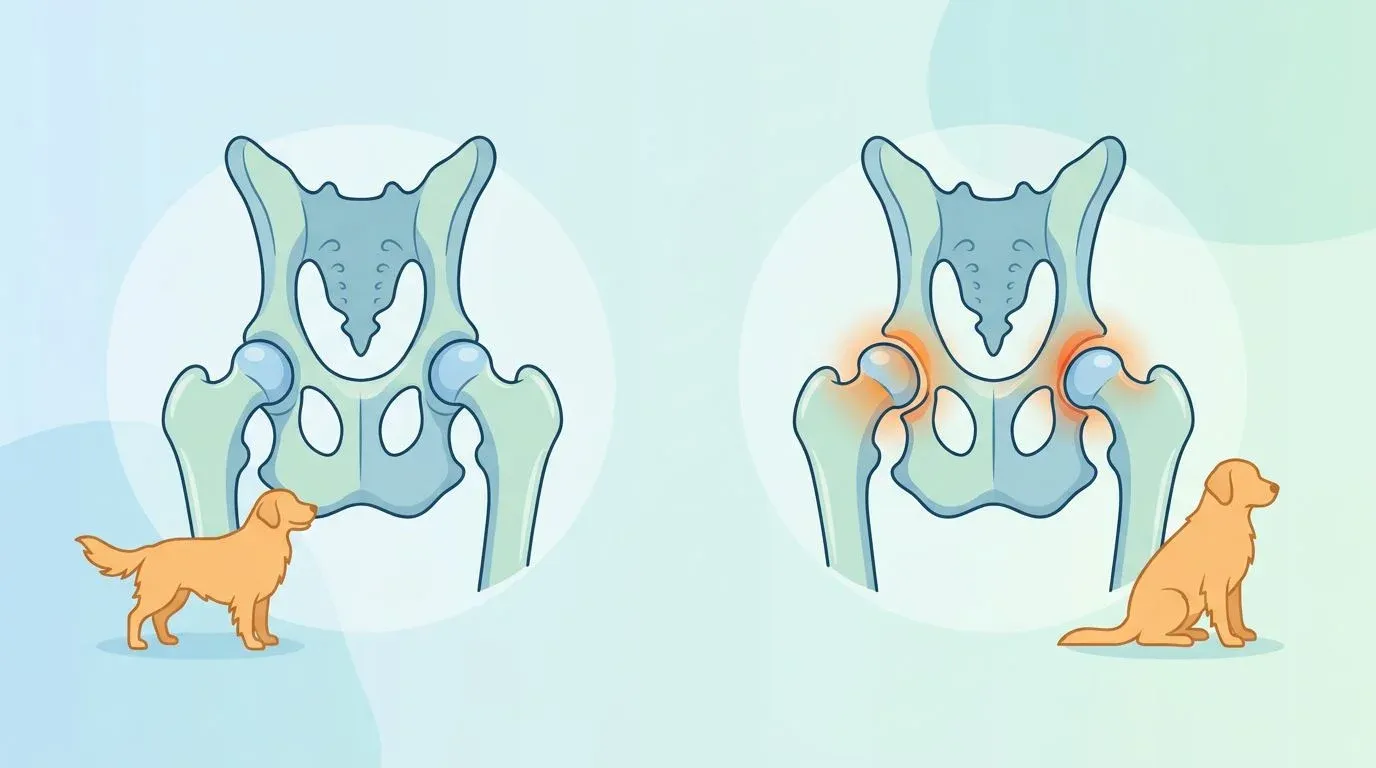
The canine hip is a ball-and-socket joint. The femoral head (the rounded top of the thigh bone) should sit snugly within the acetabulum (the cup-shaped socket in the pelvis), held in place by a tight joint capsule and a short ligament called the ligamentum teres. A layer of smooth hyaline cartilage covers both surfaces, and synovial fluid inside the joint provides lubrication and nutrition to that cartilage.
In a dog with hip dysplasia, the fit between ball and socket is loose — a condition called joint laxity. Instead of gliding smoothly, the femoral head shifts, rocks, and occasionally subluxates (partially slips out of the socket). This abnormal motion damages cartilage progressively, triggers chronic inflammation, and over time produces the bone remodeling and osteophyte formation (bone spurs) that characterize secondary osteoarthritis.
This is why “hip dysplasia” is better thought of as a developmental process rather than a static defect. A puppy with lax hips does not inevitably reach severe arthritis. How much cartilage damage accumulates depends on the degree of initial laxity, body weight, activity type, and how early management begins.
Genetic Factors and Environmental Triggers
Hip dysplasia is polygenic — it is controlled by multiple interacting genes rather than a single mutation. This makes complete elimination through selective breeding difficult, but it also means environment plays a meaningful role. Research published in the Journal of the American Veterinary Medical Association (JAVMA) has identified several environmental factors that can amplify a genetically susceptible dog’s risk:
- Rapid growth rate: Puppies fed high-calorie diets that promote faster-than-normal growth produce bone that outpaces the structural maturity of the soft tissue stabilizing the joint.
- Overfeeding: Independent of growth rate, excess body weight during puppyhood places greater mechanical stress on developing cartilage.
- High-impact exercise during development: Repetitive jumping, rough play on hard surfaces, and forced long runs before skeletal maturity stress a joint that is still consolidating.
- Slippery surfaces: Chronic micro-slipping on smooth flooring can continuously stress the joint capsule in a predisposed puppy.
Understanding these modifiable factors gives owners of at-risk breeds real preventive leverage during the critical 4–12 month developmental window.
Fact 2: Breed Risk Is Quantifiable — and the Numbers May Surprise You
High-Risk Large Breeds: Labrador, Golden Retriever, German Shepherd
The Orthopedic Foundation for Animals (OFA) maintains the world’s largest open-access orthopedic database, with hip evaluation records on over 1.4 million dogs. Their cumulative statistics reveal the breeds where hip dysplasia is most prevalent:
| Breed | OFA Dysplastic Rate (%) |
|---|---|
| Bulldog (English) | ~73% |
| Pug | ~64% |
| Dogue de Bordeaux | ~57% |
| Otterhound | ~54% |
| Neapolitan Mastiff | ~51% |
| Saint Bernard | ~47% |
| Clumber Spaniel | ~46% |
| Black and Tan Coonhound | ~26% |
| German Shepherd | ~20% |
| Golden Retriever | ~20% |
| Labrador Retriever | ~13% |
| Rottweiler | ~21% |
Source: OFA Breed Statistics, accessed 2026. Rates are cumulative across all evaluated dogs; actual rates in screened breeding populations are typically lower.
The numbers for Bulldogs and Pugs may seem counterintuitive — these are not large breeds. Their skeletal proportions, however, produce inherently abnormal hip geometry. Among working and sport breeds that owners of large dogs most commonly own, German Shepherds, Goldens, and Labs carry the largest absolute burden simply because of the sheer number of dogs in each breed population.
Why Medium and Small Breeds Aren’t Immune
Hip dysplasia affecting breeds prone to hip dysplasia is a common framing, but it creates a false sense of security for owners of medium-sized dogs. Breeds like the Chow Chow (~19%), Finnish Spitz (~19%), and even some herding breeds are meaningfully affected. Small breeds can also develop dysplasia, though at lower rates and often with milder clinical signs.
The practical implication: if your dog of any size is showing hind-end gait changes, hip dysplasia belongs on the differential diagnosis list — not only for the breeds in the table above.
Fact 3: Symptoms Follow Two Distinct Timelines
Gait Changes: Bunny Hopping, Hip Sway, Stair Avoidance
Hip dysplasia in dogs symptoms often appear through movement before they become obvious at rest. The most recognizable gait abnormality is “bunny hopping” — the dog moves both hind legs together simultaneously rather than in an alternating stride when running. This occurs because the brain compensates for painful or unstable hips by recruiting the trunk and back muscles to assist locomotion.
Other observable gait changes include:
- A wider-than-normal hind-end stance
- Swaying or rolling motion through the hips during normal walking
- Reluctance to use stairs, jump into the car, or climb onto furniture
- Visible asymmetry — one hip appears to rise higher than the other when walking
Exercise Intolerance and Stiffness on Rising
At-home observation checklist — 6 signs to watch for:
- Morning stiffness: The dog rises slowly after sleep, takes several minutes to loosen up, and may be reluctant to put full weight on the hind legs initially
- Exercise intolerance: Shorter walks, lagging behind on leash, wanting to stop and rest sooner than usual
- Difficulty rising from lying down: Pushing up unevenly, or using front legs to pull the body before the hind end follows
- Reduced range of motion: Hind leg appears stiff during extension; dog avoids hip flexion movements like squatting for elimination
- Muscle atrophy: The thigh muscles on one or both sides visually smaller than expected; hind end looks narrower than the front
- Behavioral changes: Increased irritability when touched near the hips or lower back, reluctance to be groomed in that area
These signs don’t confirm hip dysplasia — other conditions produce similar presentations. But they are clear indicators that a veterinary orthopedic evaluation is warranted.
Growing Puppy vs Adult Dog Symptoms
The clinical picture differs meaningfully between young and adult dogs:
Young dogs (5–18 months): Symptoms are driven primarily by acute joint laxity. The loose joint capsule allows excessive movement, causing pain with activity. These dogs often have periods of acute lameness after exercise, then appear normal at rest. Because this presentation can look like a muscle strain or growing pains, it is frequently underdiagnosed.
Adult and senior dogs (5+ years): Symptoms reflect accumulated secondary osteoarthritis. The joint has become “tighter” as bone remodeling has occurred, but the cartilage surface is significantly degraded. These dogs show more consistent, persistent stiffness and chronic pain — less acute-onset lameness, more gradual decline in activity level. If arthritis progresses in older dogs, pain management becomes the central goal of care.
Fact 4: Diagnosis Has Changed — PennHIP, OFA, and Standard X-Rays Are Not Equivalent
PennHIP: The Gold Standard for Early Detection (DI Explained)
PennHIP (University of Pennsylvania Hip Improvement Program) uses a three-view radiographic protocol developed by Dr. Gail Smith and colleagues, published in JAVMA in 1990. Its key innovation is the distraction view — the hips are physically distracted using a fulcrum device to maximize and measure the degree of laxity, expressed as the Distraction Index (DI).
DI ranges from 0 to 1.0:
- DI of 0 = no laxity (femoral head perfectly centered)
- DI of 0.3 or below = low risk of developing osteoarthritis
- DI above 0.7 = high risk of significant dysplasia
PennHIP can be performed as early as 16 weeks of age, making it the only method capable of informing early breeding selection decisions and allowing proactive management in high-risk puppies. The procedure requires a veterinarian certified in PennHIP technique; a list of certified practitioners is maintained at the PennHIP website.
OFA: Official Certification After Age 2
The OFA method evaluates a single ventrodorsal (extended-leg) radiograph and classifies hip conformation into seven categories: Excellent, Good, Fair (all considered Normal), Borderline, and Mild, Moderate, or Severe Dysplasia. Preliminary evaluations can be submitted before age two, but official certification requires the dog to be at least 24 months old.
For breeders using OFA certification as the gating criterion, this means no breeding decisions can be made until well into adulthood — after a dog may already have been bred once or twice.
What to Ask Your Vet
| Method | Earliest Age | What It Measures | Best For |
|---|---|---|---|
| PennHIP | 16 weeks | Distraction Index (laxity) | Early screening, breeding decisions, high-risk breeds |
| OFA | 12 months (prelim) / 24 months (official) | Hip conformation grade | Certification, breed registry requirements |
| Standard radiograph | Any age | Joint space, osteophytes, remodeling | Diagnosing clinical disease in symptomatic dogs |
When your dog is first evaluated for suspected hip dysplasia, asking specifically about PennHIP versus a standard radiograph is worthwhile. A standard radiograph in an extended-leg position can underestimate laxity and may appear relatively normal even in a dog with significant joint instability.
Fact 5: Surgery Is One Option — Not the Default Path
Conservative Management: Weight Control, Exercise Plans, Physical Therapy
Dog hip dysplasia treatment without surgery is the appropriate first approach for many dogs — particularly those with mild to moderate dysplasia, older dogs who are poor anesthetic candidates, and dogs whose pain is controlled adequately by a multimodal conservative plan. The four pillars of conservative management are:
1. Weight control. Reducing excess body weight is the single highest-impact intervention in overweight dogs. Each kilogram of excess weight applies several kilograms of additional force across the hip joint with every step. The relationship between excess body weight and joint health is well established: even modest weight loss (10–15% of body weight in overweight dogs) produces measurable improvements in pain scores and gait analysis.
2. Structured low-impact exercise. Controlled leash walks on even, non-slippery surfaces maintain muscle mass without jarring the joint. Swimming and underwater treadmill therapy (hydrotherapy) are particularly valuable because water buoyancy eliminates most of the joint load while allowing full range of motion. See the Home Care section below for a specific exercise protocol.
3. Physical therapy and rehabilitation. Canine rehabilitation practitioners (certified by organizations such as CCRT or CCRP) use therapeutic exercises, massage, and modalities including ultrasound and near-infrared therapy to reduce pain and maintain muscle function. For dogs managing hip dysplasia long-term, periodic professional rehabilitation sessions can reset muscle imbalances that develop as the dog compensates around the painful joint. Near-infrared therapy works by delivering photons to deeper tissues, which promotes cellular energy production and has been shown in animal studies to reduce joint inflammation and support tissue recovery.
4. Pharmacologic management. NSAIDs (non-steroidal anti-inflammatory drugs) prescribed by a veterinarian remain the backbone of medical pain management. Additional options include gabapentin, amantadine, and injectable polysulfated glycosaminoglycan (Adequan), which has demonstrated slowing of cartilage degradation in veterinary studies.
Surgical Options: JPS, TPO, FHO, THR Compared
Dog hip dysplasia surgery options fall into two categories: procedures that alter joint mechanics to prevent progression (appropriate for young dogs) and salvage procedures that eliminate painful joint contact (appropriate for dogs with significant arthritis).
| Procedure | Full Name | Age / Indication | Estimated Cost (USD) | Recovery |
|---|---|---|---|---|
| JPS | Juvenile Pubic Symphysiodesis | Under 5 months, at-risk puppies | $1,000–$2,500 | 4–6 weeks |
| TPO | Triple Pelvic Osteotomy | 5–10 months, before arthritis | $3,000–$6,000 (bilateral) | 8–12 weeks |
| FHO | Femoral Head Ostectomy | Any age, severe arthritis | $1,500–$3,500 per hip | 3–4 months |
| THR | Total Hip Replacement | Over 9–12 months, severe arthritis | $4,500–$7,000 per hip | 8–12 weeks |
Cost ranges are estimates for the continental US and vary significantly by region, clinic type, and whether CT planning is required. Pet insurance may cover a substantial portion of orthopedic surgery costs; verify whether your policy covers congenital/hereditary conditions and their onset-of-symptoms timing requirements.
Brief notes on each:
- JPS is a minimally invasive procedure that fuses the pubic symphysis in very young puppies, causing the acetabulum to rotate outward and improve coverage. It must be performed before the pelvis has finished forming — typically before 5 months.
- TPO redirects the socket around the femoral head through three cuts in the pelvis. It is appropriate when there is significant laxity but the cartilage surface remains largely intact.
- FHO removes the femoral head entirely, allowing a fibrous “false joint” to form. It is a cost-effective salvage option with good outcomes in small-to-medium dogs; outcomes in large breeds over 50 lbs (23 kg) are less consistent.
- THR replaces both joint surfaces with prosthetic components and can restore near-normal function in appropriately selected patients. It carries the highest cost and the most demanding postoperative protocol, but outcomes data from veterinary centers are very positive.
Surgery vs Conservative: A Decision Framework
Most veterinary orthopedic specialists use the following general framework when discussing surgical options with owners. The right path is always an individualized conversation with a board-certified veterinary surgeon (Diplomate ACVS):
- Young dog (<12 months) + significant laxity confirmed + no/minimal arthritis → JPS or TPO likely appropriate; these windows close
- Young to middle-aged dog + moderate-to-severe pain + inadequate response to conservative care for 4–6 weeks → THR or FHO worth serious consideration
- Older dog + stable on conservative management + acceptable quality of life → continue and optimize conservative plan
- Any dog + owner cost or health constraints preclude surgery → maximize conservative care; FHO as future fallback if pain escalates
If your dog has been diagnosed with hip dysplasia and you’re uncertain which path is appropriate, seeking a consultation with a board-certified veterinary surgeon is worthwhile. Many university veterinary teaching hospitals offer specialist consultations at accessible price points.
Fact 6: Home Care Is Where Daily Outcomes Are Actually Decided
Weight Management: Setting Goals with BCS
Body Condition Score (BCS) is a 9-point scale used to assess whether a dog is underweight, ideal, or overweight by evaluating rib palpability, waist definition, and abdominal tuck. For dogs with hip dysplasia, maintaining a BCS of 4–5 (ideal) is a genuine therapeutic goal — not just a wellness recommendation.
Practical steps:
- Ask your veterinarian to assign a current BCS at each visit
- Use a feeding guide calibrated to ideal body weight, not current body weight
- Weigh food portions with a kitchen scale; “cup” measurements vary widely
- Treats count — factor them into the daily calorie budget
- Reweigh monthly; aim for 0.5–1% body weight loss per week if actively reducing
Keeping a dog with hip dysplasia lean also protects against secondary injuries. Hip instability creates an unusual gait pattern that transfers abnormal stress to the stifle (knee) joint, which is one reason why cruciate ligament tears are more common in dogs with underlying hip pathology.
Joint-Friendly Environment: Flooring, Beds, Ramps
The home environment for a dog with hip dysplasia needs to reduce the number of moments per day where the joint is stressed unexpectedly:
- Flooring: Hardwood, tile, and vinyl are slippery. Area rugs with non-slip backing on primary walking routes, especially where the dog rises and approaches food/water bowls, provide meaningful traction. Rubber-backed yoga mats are an affordable solution for specific problem areas.
- Bedding: Orthopedic memory foam beds reduce the pressure of lying on hard floors and make rising easier. Position beds away from drafty areas — cold makes stiff joints stiffer.
- Ramps and steps: Pet ramps for the car, couch, and bed reduce the daily impact of jumping and are particularly valuable for large dogs. Introduce the ramp gradually with positive reinforcement.
- Water and food bowl height: Elevated bowls (positioned so the dog can eat and drink without significant neck or hip flexion) reduce postural strain during meals.
This kind of environmental management is also central to caring for senior dogs with ongoing joint disease, where cumulative daily stress on joints determines long-term comfort.
Recommended Exercises and Activities to Avoid
Beneficial exercises for hip dysplasia dog home care:
| Exercise | Notes |
|---|---|
| On-leash walks (flat surface) | 2–3 short sessions (10–15 min) preferred over one long session; avoids fatigue-related gait compensation |
| Swimming | Excellent; eliminates joint load while maintaining full range of motion and muscle mass |
| Underwater treadmill (hydrotherapy) | Best outcome when supervised by a rehabilitation professional |
| Gentle hill work (uphill only) | Activates glute and hamstring muscles that support the hip; avoid steep grades |
| Cavaletti poles (low, slow) | Encourages conscious limb placement and hip flexion; can be done at home with PVC pipe |
| Balance/proprioception exercises | Standing on a balance disc or cushion (supervised); builds stabilizing musculature |
Activities to avoid or modify:
- Jumping on/off furniture or into vehicles without ramp assistance
- Rough play with other dogs involving twisting, jumping, and rapid direction changes
- Sustained running on hard surfaces (pavement)
- Fetch involving high-speed direction changes and abrupt stops
- Forced exercise when the dog is visibly stiff (immediately after rest)
If a dog shows increased limping for more than 24 hours after an activity, that activity was too much. The general principle: if the dog is worse the following morning, reduce intensity. If the dog improves gradually over a week of structured activity, you’ve found a sustainable level.
Hind-limb gait abnormalities that look similar to hip dysplasia can also originate from patellar problems — if your dog’s gait changes involve the kneecap skipping or locking, patellar luxation is an important condition to distinguish from hip pathology with a proper orthopedic examination.
FAQ
Is hip dysplasia in dogs genetic?
At what age do hip dysplasia symptoms appear in dogs?
Can dogs live comfortably with hip dysplasia without surgery?
Do joint supplements help dogs with hip dysplasia?
What is the difference between PennHIP and OFA for diagnosing hip dysplasia?
Related Articles
The Hidden Link Between Your Dog's Weight and Joint Health
Extra weight does far more than strain your dog's joints — it actively inflames them. Learn the dual-pathway science and a practical roadmap to protect joint health.
Dog Arthritis: Symptoms and Management
Recognize early signs of arthritis in dogs and learn effective management strategies for pain relief and improved mobility.
Complete Guide to Patellar Luxation in Dogs
Learn about the causes, symptoms, grades, treatment options, and prevention of patellar luxation in dogs.
Is Your Dog Showing Signs of IVDD? Symptoms, Stages, and What to Do
Learn to recognize IVDD in dogs symptoms by grade and spinal region, understand treatment options from conservative care to surgery, and manage recovery at home.
Dog Cruciate Ligament Tear: 7 Things Every Owner Must Know
Dog cruciate ligament tear guide: recognize symptoms, compare TPLO vs TTA surgery, follow a phased recovery timeline, and protect the opposite knee.